DEEP VEIN THROMBOSIS (DVT)
DEEP VEIN THROMBOSIS (DVT): UNDERSTANDING THE RISKS
When blood clots form in deep leg veins, quick recognition and treatment are crucial. As The Leg Vein Experts, we provide comprehensive evaluation and urgent care for DVT to prevent serious complications.

UNDERSTANDING DEEP VEIN THROMBOSIS
QUESTIONS & ANSWERS
WHAT CAUSES DEEP VEIN THROMBOSIS?
Deep vein thrombosis (DVT) occurs when blood clots form in deep leg veins. While it can affect anyone at any age, certain factors increase your risk:
- Slow Blood Flow
- Heart conditions
- Limited mobility
- Extended travel
- Prolonged bed rest
- Weight factors
- Tissue Trauma
- Recent injuries
- Surgical procedures
- Significant bruising
- Blood Composition Changes
- Inherited clotting disorders
- Family history
- Certain medications
- Inflammatory conditions
Expert Insight: Understanding your risk factors is crucial for prevention. Many DVT cases can be prevented with appropriate precautions and early intervention.
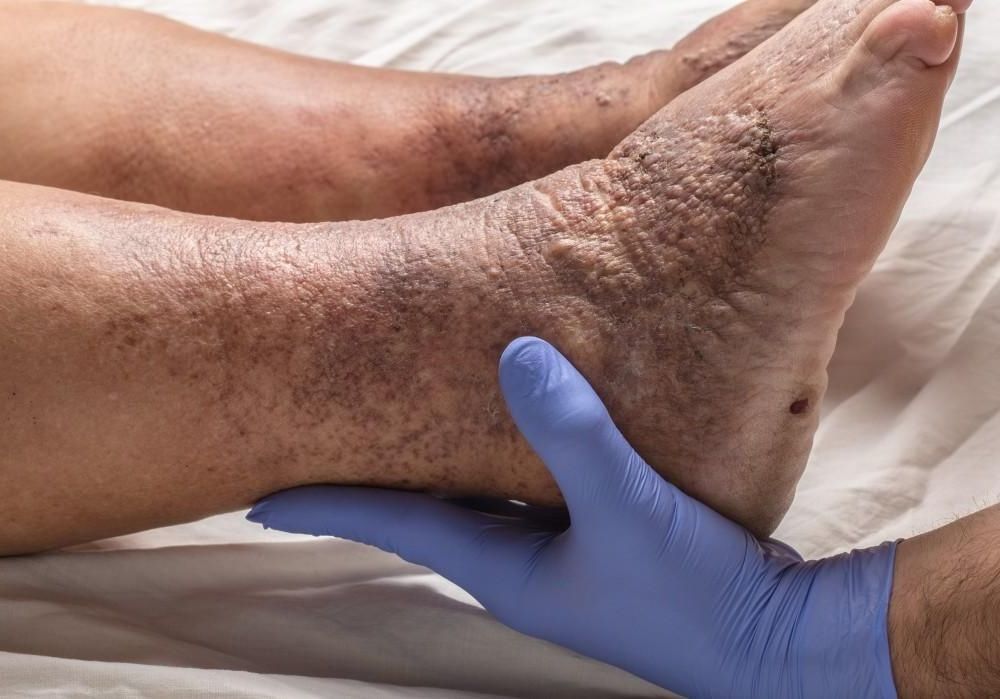
WHAT SYMPTOMS SHOULD I WATCH FOR?
DVT can present differently in each person:
Common Signs:
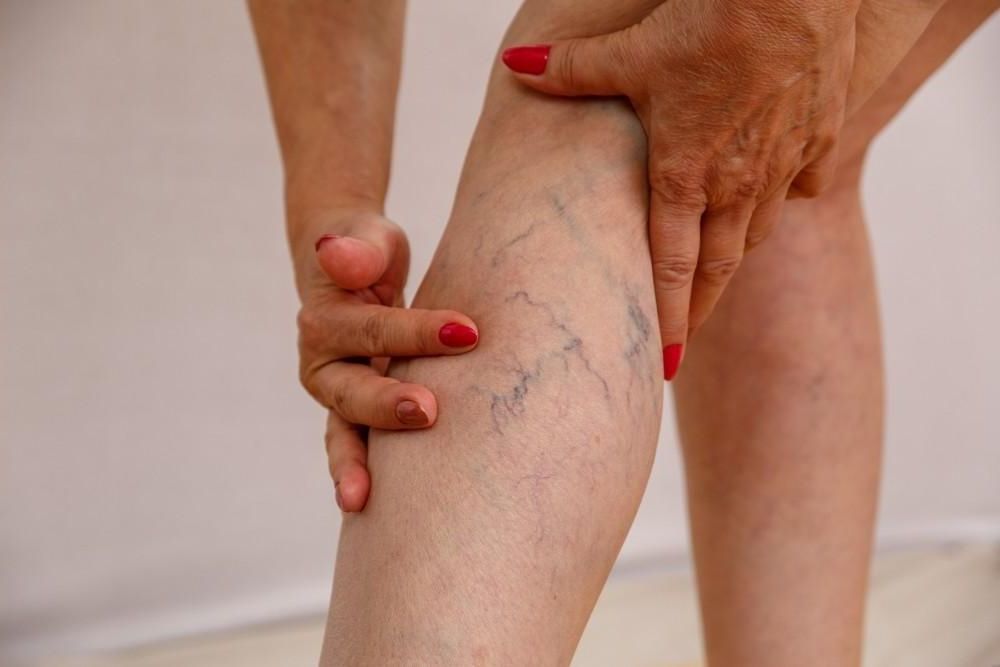
- Leg pain (ranging from mild to severe)
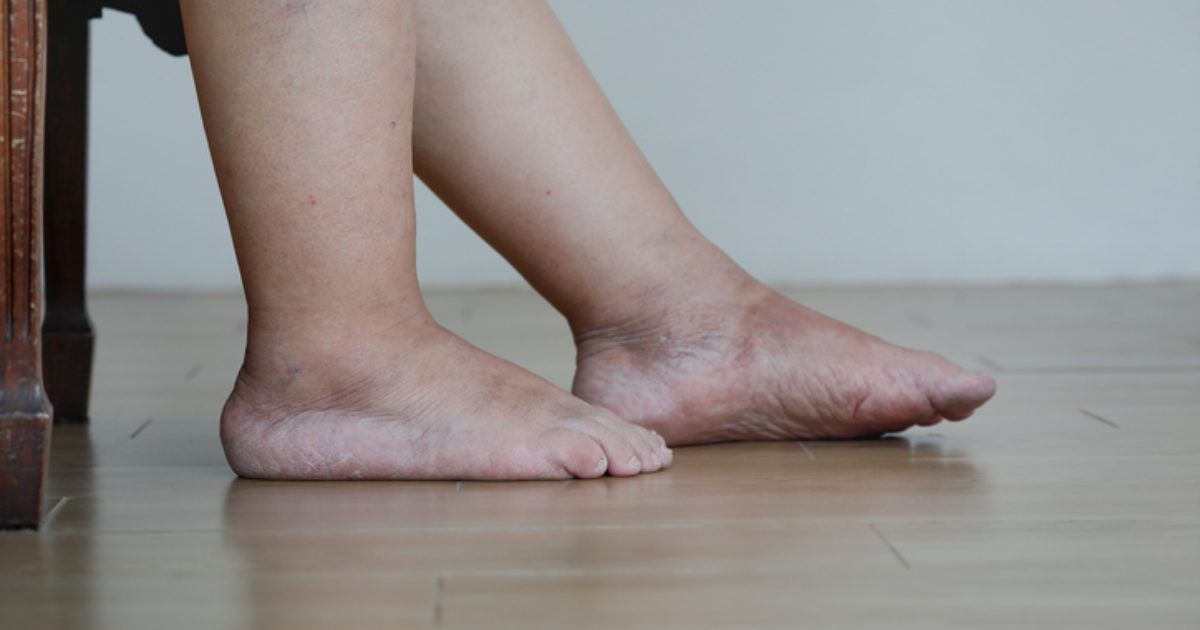
- Sudden leg swelling
- Warmth in one leg
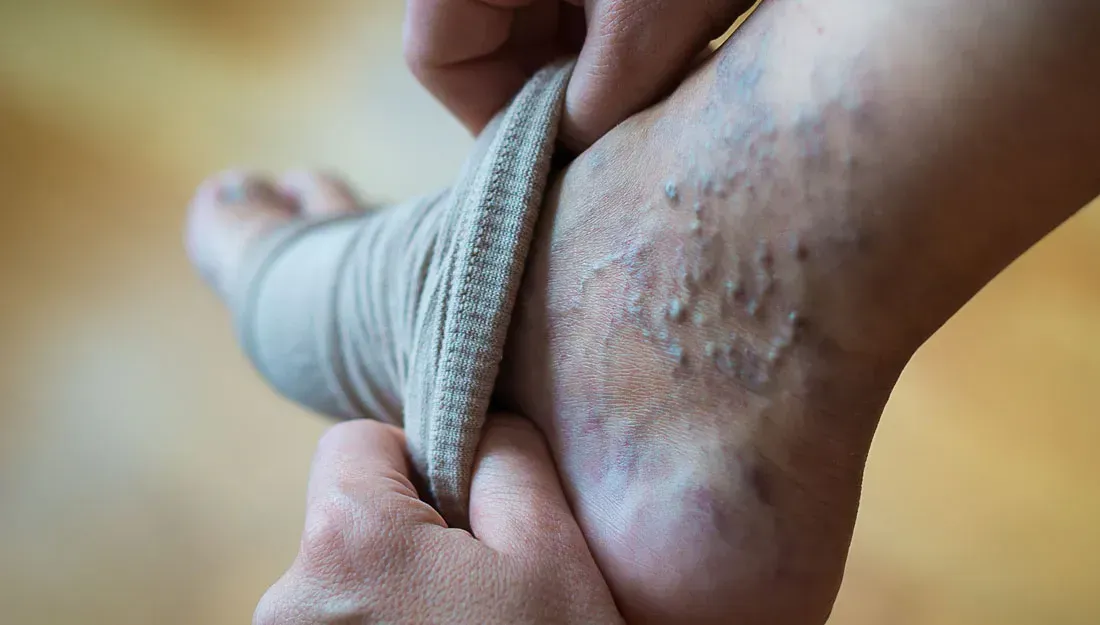
- Skin color changes
Warning Signs of Complications:
- Unexplained shortness of breath
- Chest discomfort
- Unusual cough
- Rapid heartbeat
Expert Insight: Some people may not experience obvious symptoms initially. Any sudden leg swelling or unexplained leg pain deserves immediate medical attention.
HOW IS DEEP VEIN THROMBOSIS DIAGNOSED AND TREATED?
At Vascular Solutions, we understand that every patient's vein condition is unique. Our treatment approach begins with a thorough evaluation to determine the most effective solution for your specific needs. While some patients may benefit from conservative measures like leg elevation and compression therapy, many require more advanced interventions for lasting relief.
STATE-OF-THE-ART SOLUTIONS
Our comprehensive treatment options include:
- VenaSeal® - Advanced Adhesive Treatment: A revolutionary approach using medical-grade adhesive to instantly seal affected veins. This painless procedure requires minimal recovery time, allowing you to return to your daily activities immediately.
- Radiofrequency Ablation - Precision Heat Therapy (Venclose, ClosureFast): This minimally invasive procedure uses controlled radiofrequency energy to seal problematic veins. Blood naturally redirects to healthy veins, reducing pressure and improving circulation. Most patients experience significant symptom relief within weeks.
- Varithena® - Specialized Foam Treatment: This versatile solution uses an advanced microfoam to treat veins of various sizes and locations. The foam adapts to your vein structure, effectively treating even complex vein patterns and providing comprehensive results.
- Sclerotherapy Medical - Precision Vein Treatment: This proven treatment uses specialized medications precisely injected to target and close unwanted veins. The carefully selected solution works with your body's natural processes to effectively treat spider veins and small varicose veins, gradually fading them from view while improving overall vein health.
CONSERVATIVE MEASURES (where appropriate):
- Leg Elevation
- Medical Grade Compression Hose
- Velcro Compression Wrap
- Non-Pneumatic Compression Device
- Vein Formula (Supplement)

TAKE IMMEDIATE ACTION
Don't wait if you suspect DVT. Schedule an urgent evaluation with Charlotte's trusted leg vein experts. Quick action can prevent life-threatening complications.