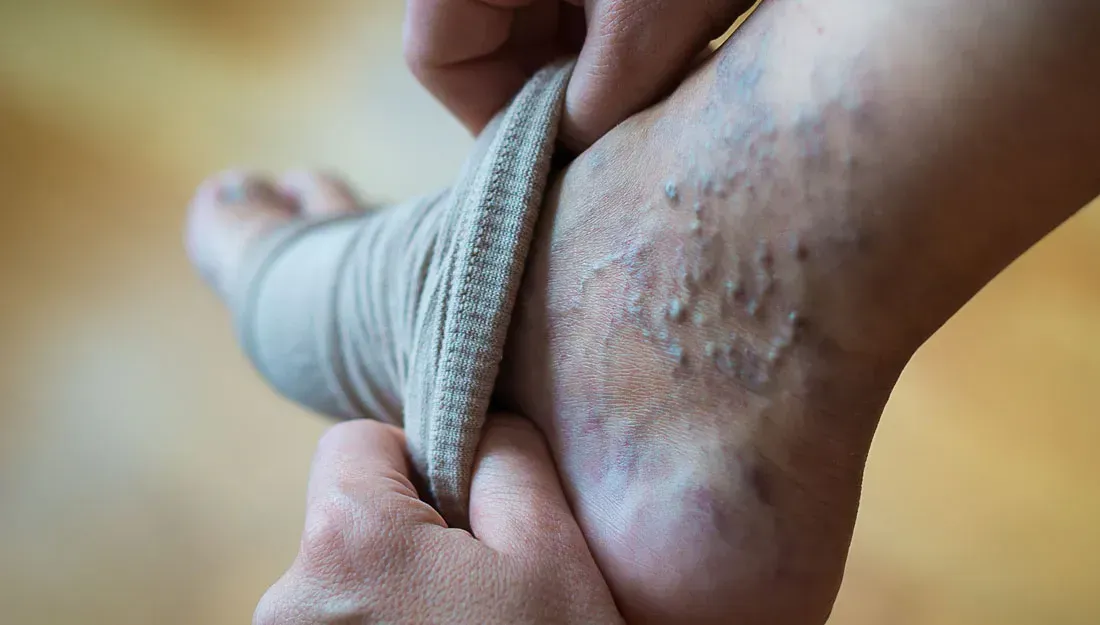
VARICOSE VEINS
VARICOSE VEIN SOLUTIONS
Living with varicose veins can be more than just a cosmetic concern – they can cause discomfort, affect your daily activities, and impact your confidence. As The Leg Vein Experts, we understand that each case is unique and requires personalized care.
EXPERT CARE YOU CAN TRUST
At Vascular Solutions, we combine advanced treatments with genuine care to solve your varicose vein problems. Led by board-certified vascular surgeon Dr. Ford, our team offers state-of-the-art solutions including:
- Radiofrequency Ablation treatment
- VenaSeal® medical adhesive system
- Varithena® foam therapy
Each minimally invasive procedure is precisely selected and customized to deliver the best possible results for your specific condition. Our approach focuses not just on improving the appearance of your legs, but on restoring healthy circulation and providing long-lasting relief.

VARICOSE VEINS
QUESTIONS & ANSWERS
WHAT CAUSES VARICOSE VEINS?

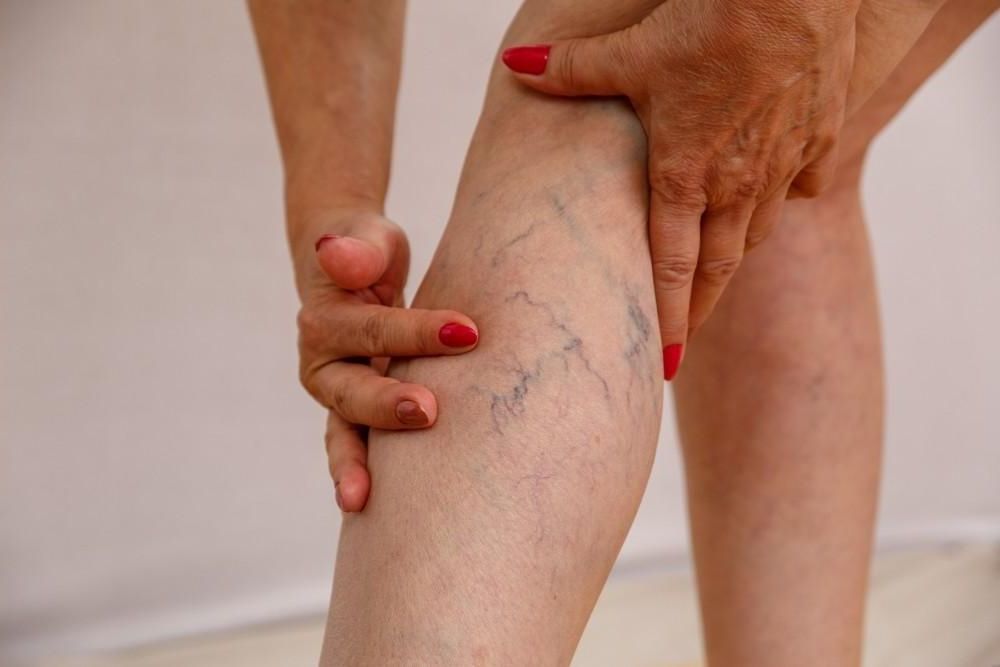
Your leg veins work continuously to move blood back to your heart, using special one-way valves to prevent backward flow. When these valves become weak or damaged, blood can flow backwards and pool in the veins, causing increased pressure. This pressure, combined with factors like aging or genetics, can cause veins near the surface to become enlarged and twisted, taking on the characteristic dark purple or blue appearance of varicose veins.
WHAT SYMPTOMS DEVELOP DUE TO VARICOSE VEINS?
While some people may not experience discomfort, varicose veins often cause:
- Aching or throbbing legs
- Evening fatigue
- Nighttime leg cramping
- Restless legs
- Persistent itching
- Burning sensations
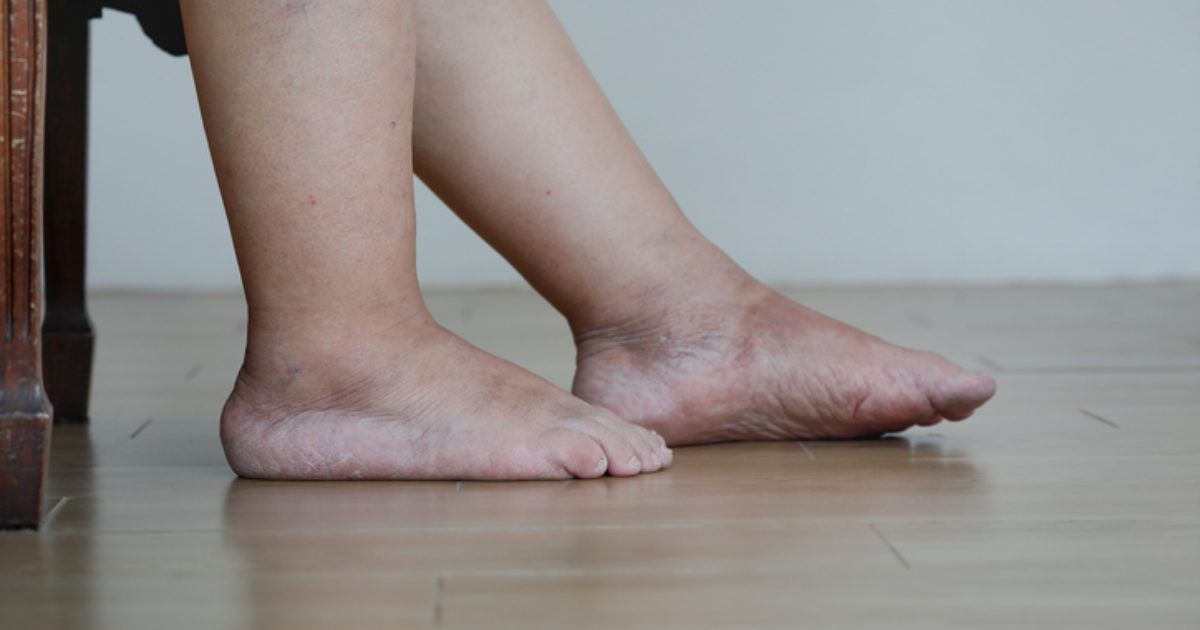
- Lower leg swelling
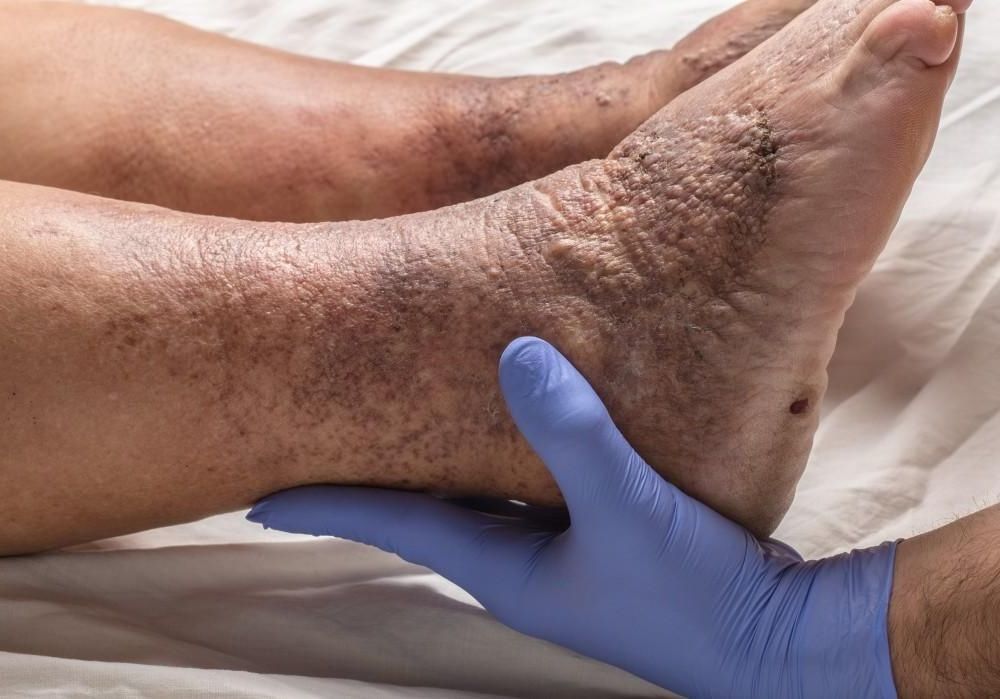
- Skin changes around the ankles
Expert Insight: Without proper treatment, varicose veins can progress to more serious conditions. Changes in skin color or texture around the ankles often signal advancing vein disease that needs medical attention.
WHAT TREATMENT OPTIONS DO I HAVE FOR VARICOSE VEINS?
At Vascular Solutions, we understand that every patient's vein condition is unique. Our treatment approach begins with a thorough evaluation to determine the most effective solution for your specific needs. While some patients may benefit from conservative measures like leg elevation and compression therapy, many require more advanced interventions for lasting relief.
STATE-OF-THE-ART SOLUTIONS
Our comprehensive treatment options include:
- VenaSeal® - Advanced Adhesive Treatment: A revolutionary approach using medical-grade adhesive to instantly seal affected veins. This painless procedure requires minimal recovery time, allowing you to return to your daily activities immediately.
- Radiofrequency Ablation - Precision Heat Therapy (Venclose, ClosureFast): This minimally invasive procedure uses controlled radiofrequency energy to seal problematic veins. Blood naturally redirects to healthy veins, reducing pressure and improving circulation. Most patients experience significant symptom relief within weeks.
- Varithena® - Specialized Foam Treatment: This versatile solution uses an advanced microfoam to treat veins of various sizes and locations. The foam adapts to your vein structure, effectively treating even complex vein patterns and providing comprehensive results.
- Phlebectomy - Precise Vein Removal: Using tiny, cosmetically-placed openings, this technique allows for direct removal of visible varicose veins through a minimally invasive approach.
- Sclerotherapy Medical - Precision Vein Treatment: This proven treatment uses specialized medications precisely injected to target and close unwanted veins. The carefully selected solution works with your body's natural processes to effectively treat spider veins and small varicose veins, gradually fading them from view while improving overall vein health.
CONSERVATIVE MEASURES (where appropriate):
- Leg Elevation
- Medical Grade Compression Hose
- Velcro Compression Wrap
- Non-Pneumatic Compression Device
- Vein Formula (Supplement)
WHAT DOES A TREATMENT PLAN LOOK LIKE?
CUSTOMIZED CARE APPROACH
Your treatment plan may combine multiple approaches for optimal results. Our board-certified specialists carefully select the most appropriate treatments based on:
- Your specific vein patterns
- Severity of symptoms
- Lifestyle needs
- Overall health goals
Expert Insight: Many patients benefit from a combination of treatments that both reduce pressure in the deeper veins and address visible surface veins. This comprehensive approach helps ensure long-lasting results.

TAKE THE FIRST STEP
Schedule your consultation today to discover which treatment options are right for you. At Vascular Solutions, we combine advanced technology with expertise to help you achieve healthier, more comfortable legs.