CONDITIONS
THE
LEG VEIN EXPERTS
COMPREHENSIVE VEIN CARE: CONDITIONS WE TREAT
At Vascular Solutions, our board-certified vascular surgeons diagnose and treat the full spectrum of vein conditions, from cosmetic concerns to complex vascular issues. As The Leg Vein Experts, we understand that vein disease can significantly impact your quality of life. Whether you're experiencing discomfort from varicose veins, concerned about spider veins, or dealing with more serious vascular conditions, our team provides expert evaluation and personalized treatment plans using the most advanced techniques available.
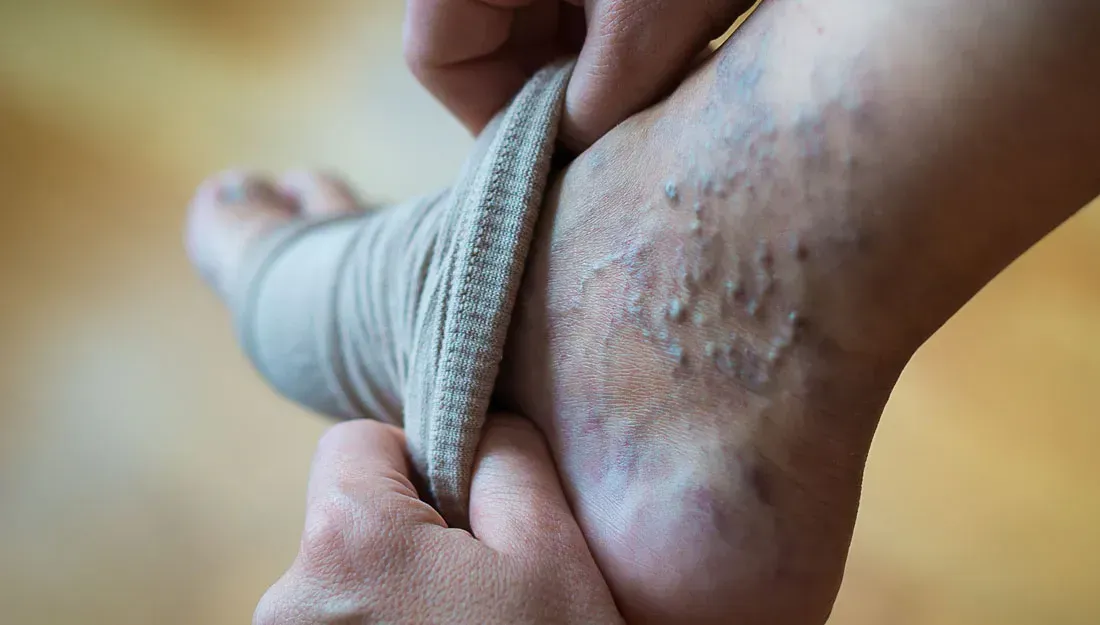
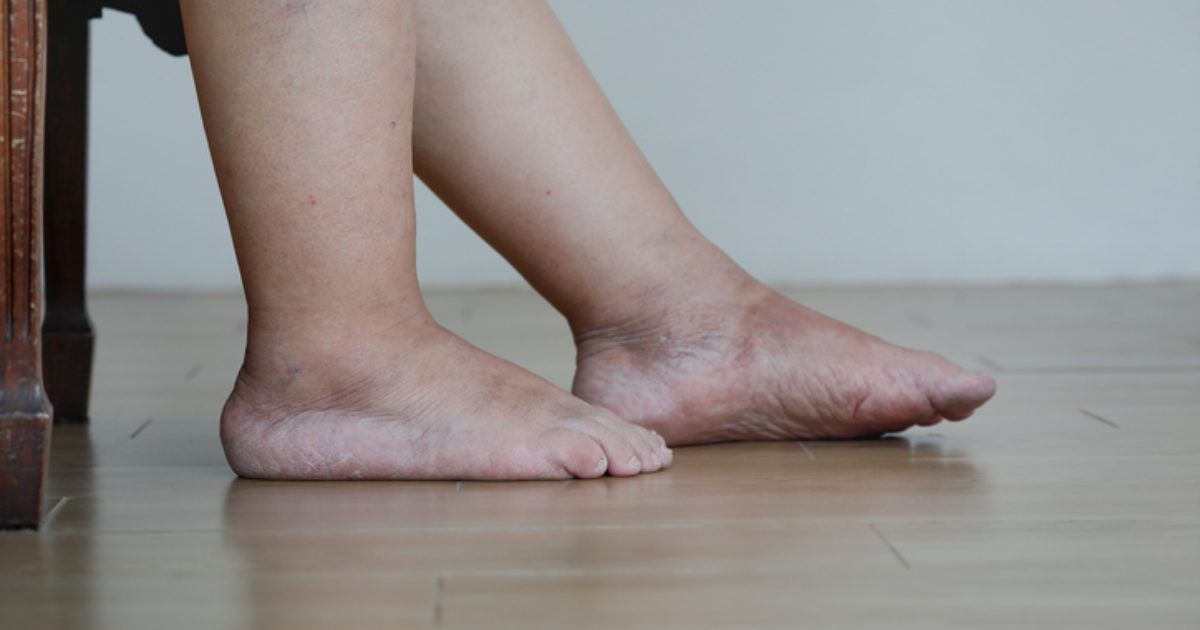
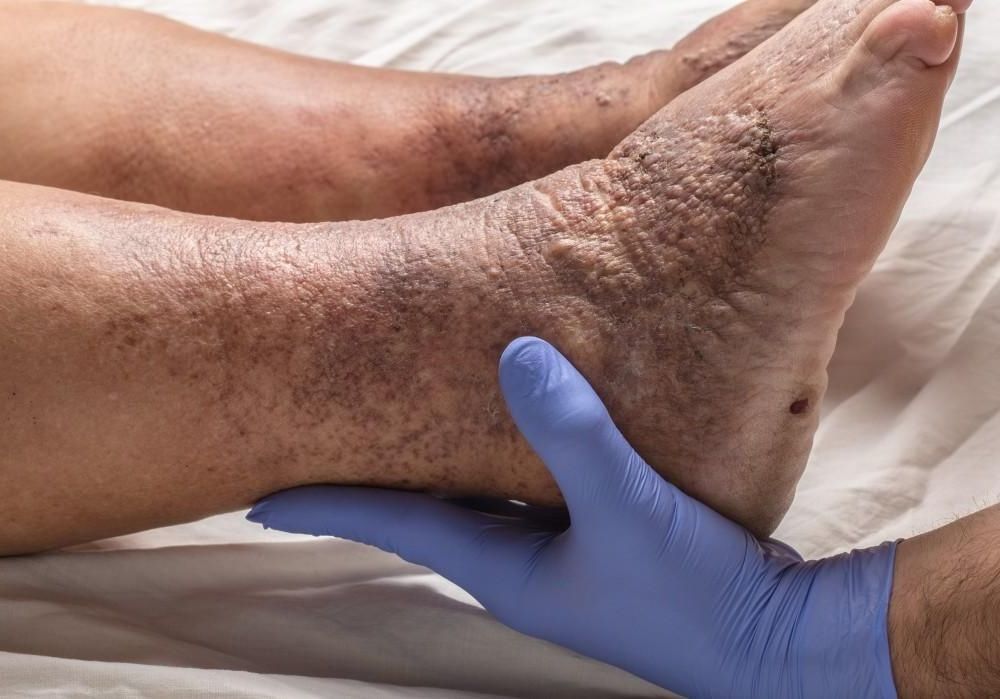
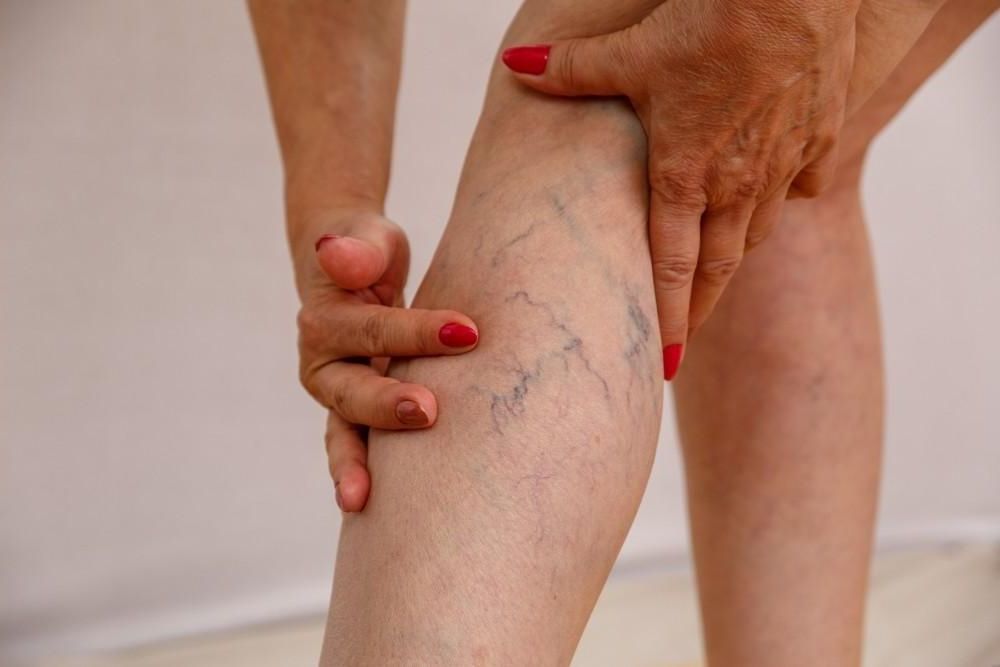
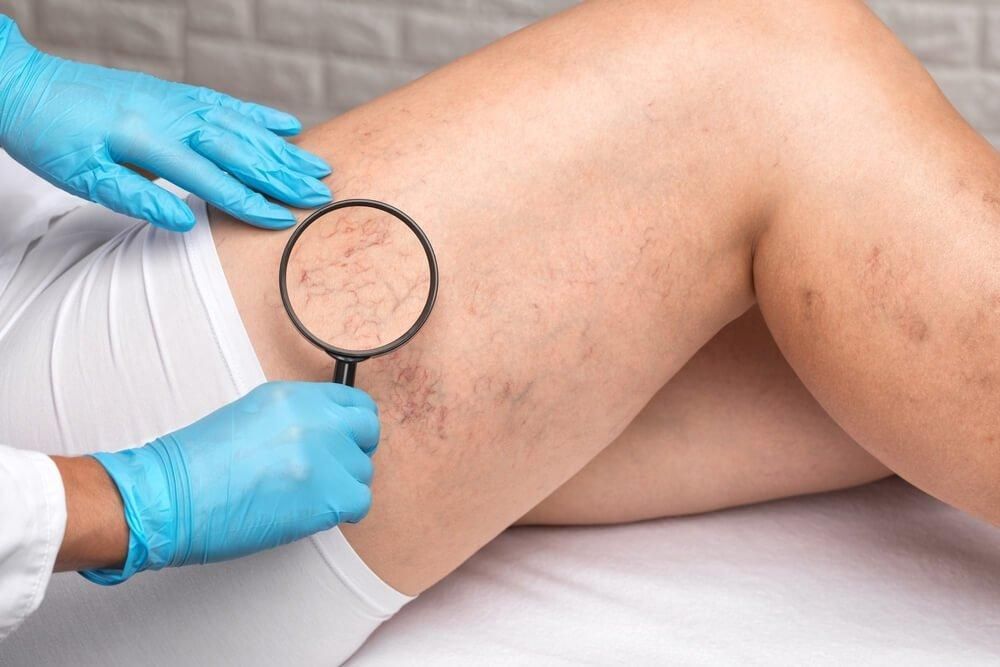
UNDERSTANDING LEG VEIN DISEASE
The underlying cause of vein disease is poor circulation, which results in blood pooling in veins, leading to increased pressure and bulging. Various factors can contribute to this condition, including genetics, age, pregnancy, obesity, and prolonged standing or sitting.
Expert Insight: You're not alone – leg vein disease affects 1 in 2 women and 1 in 3 men in the United States. Despite how common these conditions are, many people delay seeking treatment. Our experience shows that early evaluation and treatment by a vein specialist leads to better outcomes and helps prevent more serious problems from developing.

COMMON CONDITIONS:
WHY EARLY TREATMENT MATTERS
Vein disease is progressive, meaning symptoms can worsen over time if left untreated. However, there's good news - with early intervention from our board-certified specialists, most patients experience relief in as little as one week. At Vascular Solutions, we offer today’s most advanced, minimally invasive treatments:
- Customized Treatment Plans
- Non-Invasive Options
- Quick, In-Office Procedures
- Minimal Recovery Time
- Long-Term Results

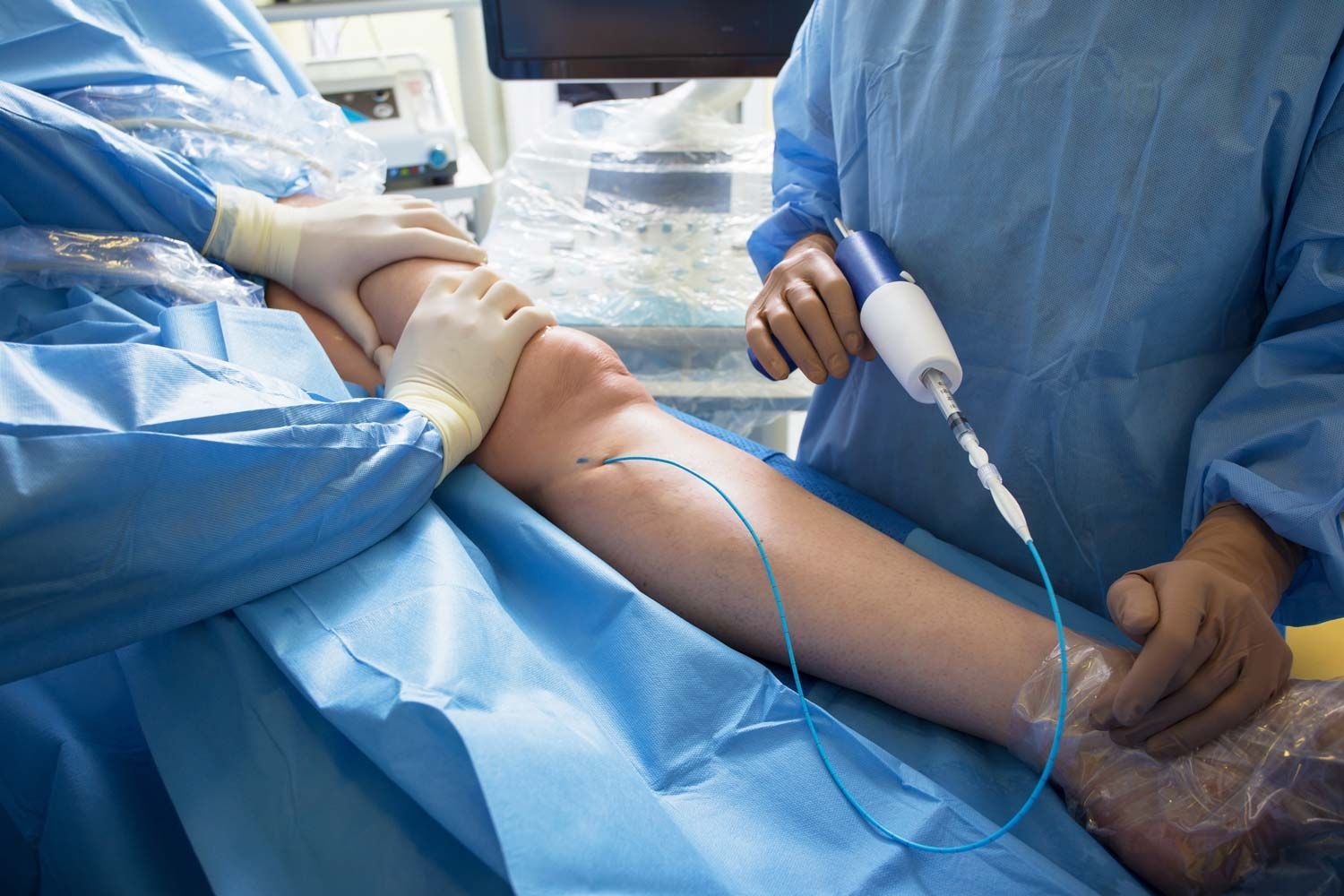
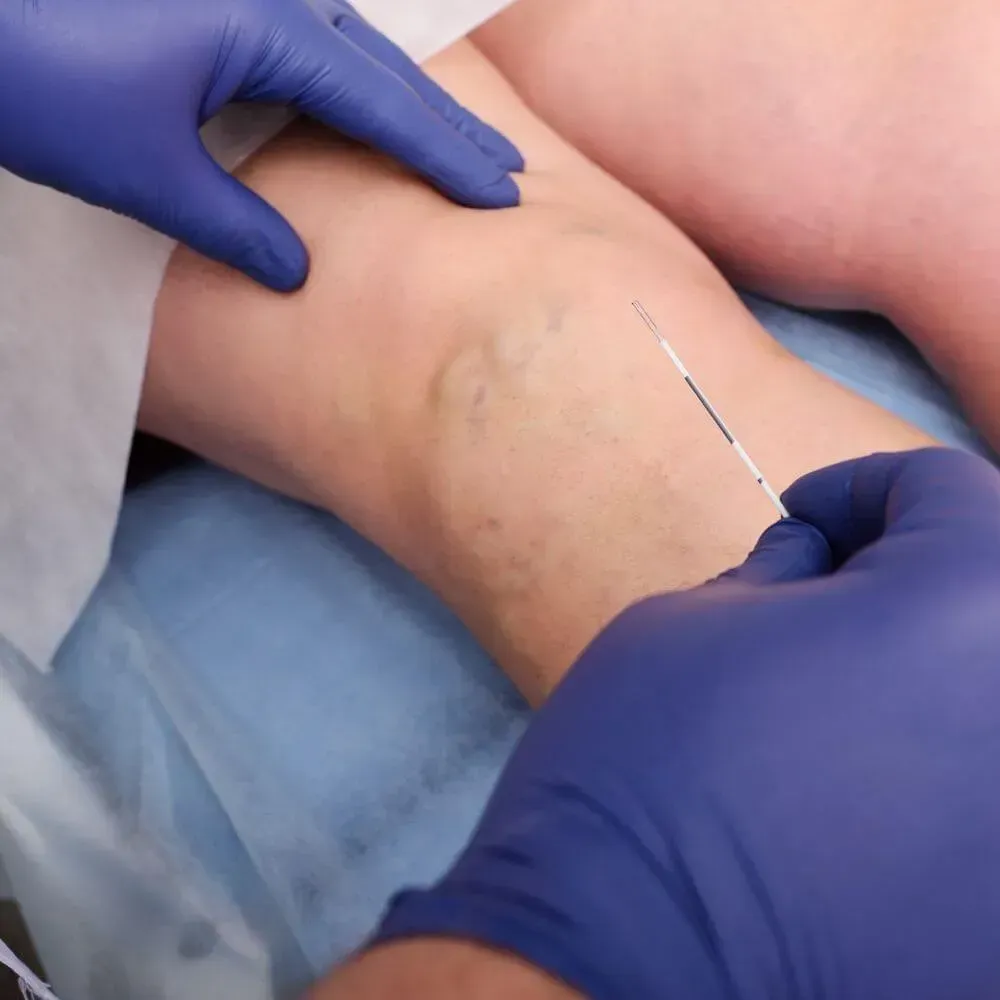
ADVANCED TREATMENT OPTIONS:
TAKE THE NEXT STEP
Contact us to schedule an evaluation today. At Vascular Solutions, we combine medical excellence with genuine care to help you achieve happier and healthier legs.