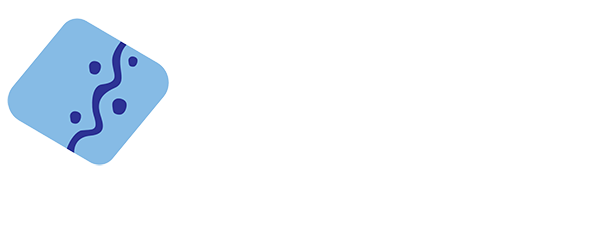TREATMENTS
THE
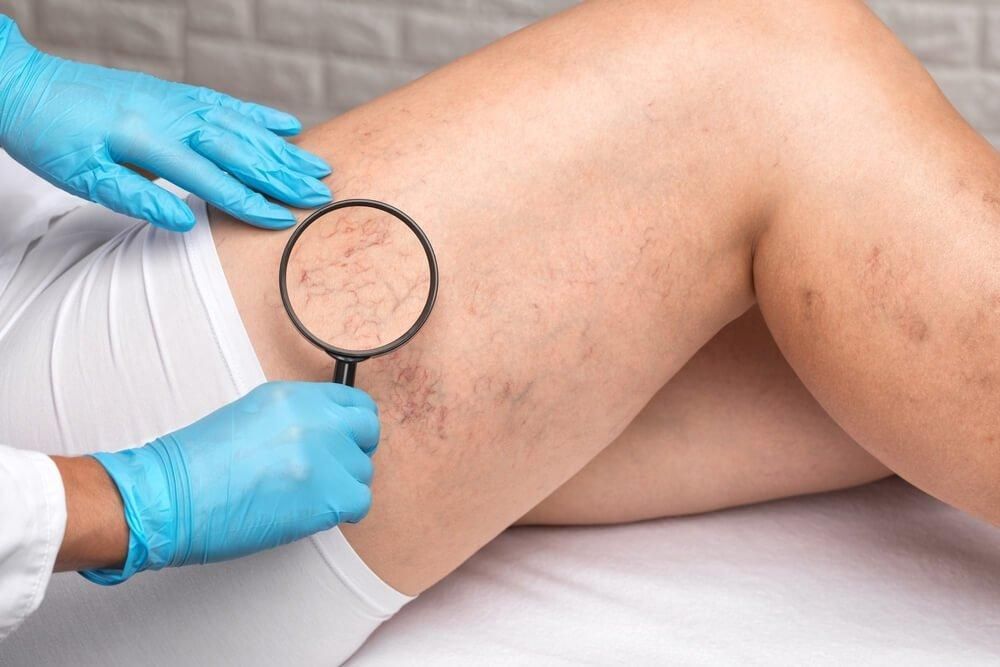
LEG VEIN EXPERTS
ADVANCED VEIN TREATMENTS: PERSONALIZED CARE FOR LASTING RESULTS
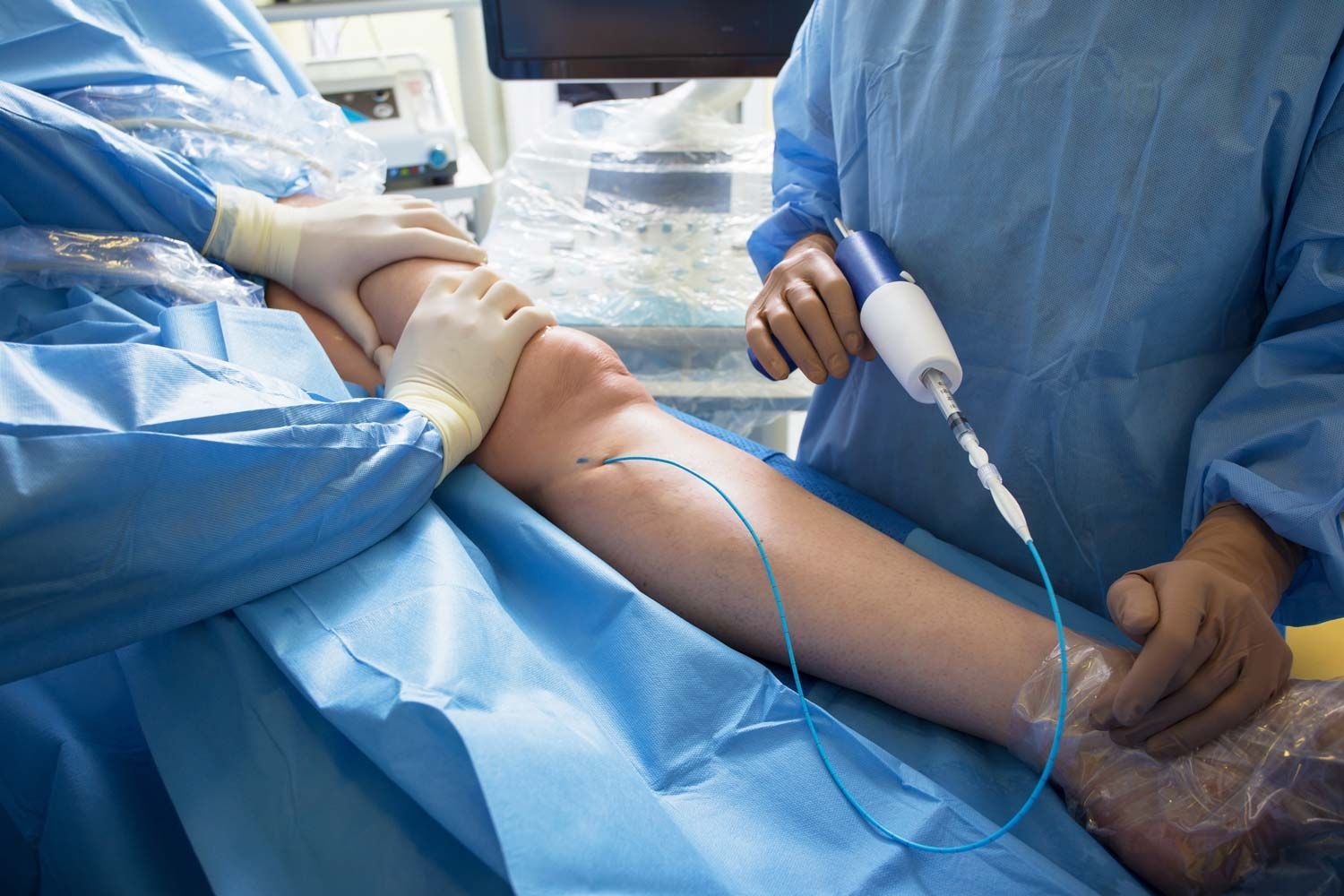
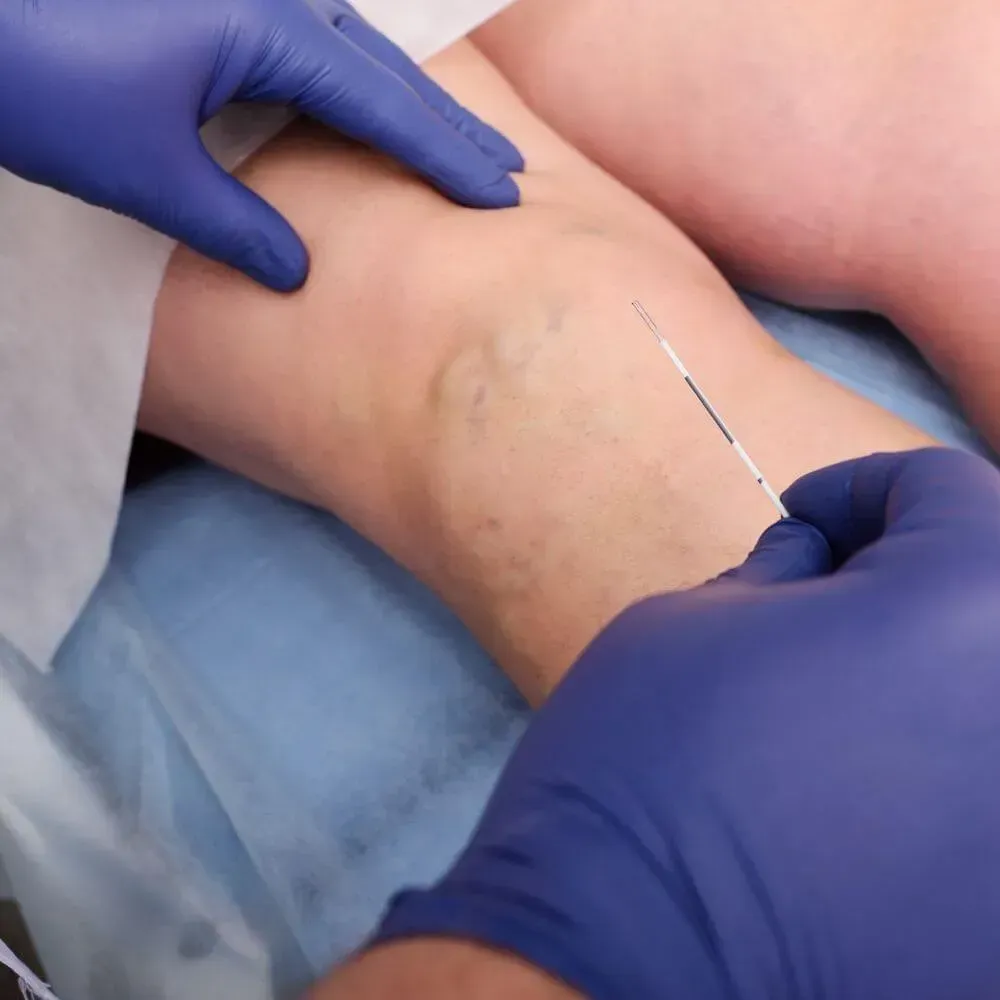
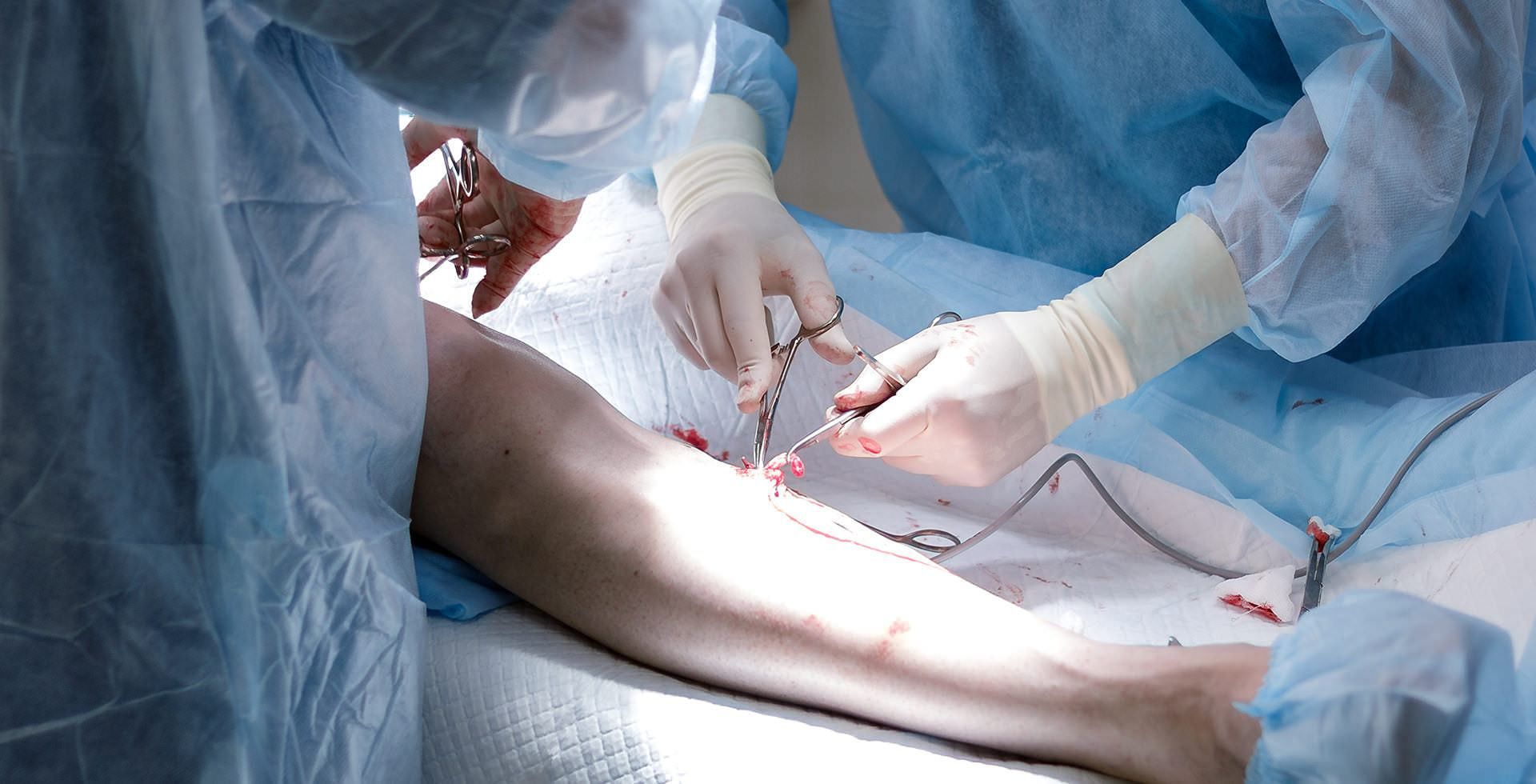
At Vascular Solutions, we offer a comprehensive range of state-of-the-art vein treatments, each carefully selected to provide optimal results with minimal downtime. Led by board-certified vascular surgeon Dr. Peter Ford and our expert vascular team, we precisely match each patient with the most appropriate treatment approach, considering factors like severity of symptoms, vein location and size, and lifestyle needs. From innovative non-thermal solutions to advanced laser procedures, we utilize the latest technologies while maintaining the highest standards of safety and effectiveness.