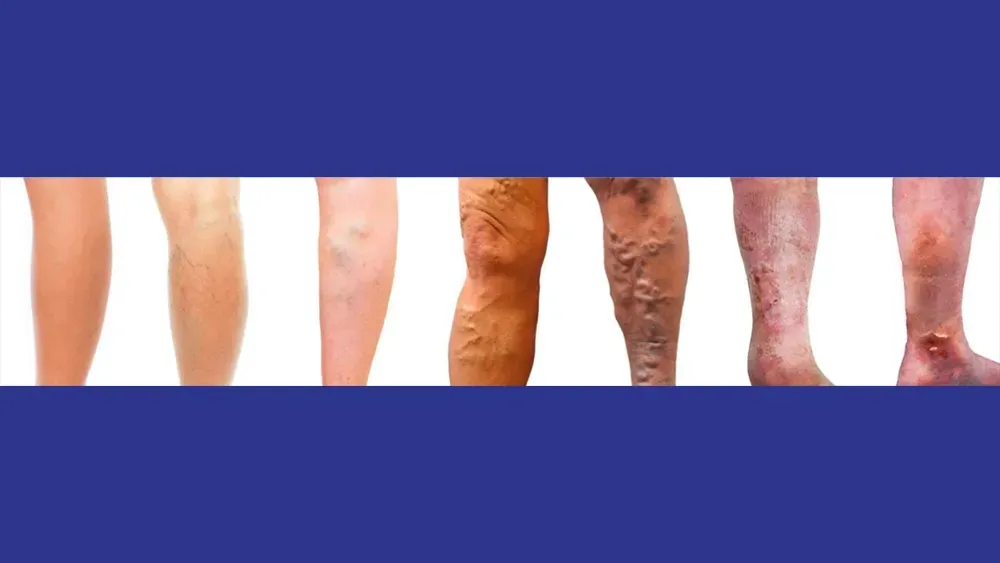
You're So Vein, You Probably Think This Song Is About You
Do you have unexplained leg pain? Do you have scattered veins on your legs? This article will explore the ways that varicose veins and vein problems can affect your legs.
LEG CIRCULATION ANATOMY:
The pipes that carry oxygen-rich blood to the tissues are called arteries. The pipes that carry oxygen-depleted blood back to the heart are called veins.
As arteries travel down the legs they branch, then repeatedly sub-branch, until eventually, the oxygen-rich blood flows through tiny, microscopic pipes called capillaries. At the level of the capillaries, oxygen is delivered to the tissues.
Capillaries are present in all living tissues including the skin, fatty tissues underneath the skin, and muscles of the legs. Once oxygen has been delivered the blood starts its journey back to the heart.
The outflow passageways of capillaries merge/join, then join again. With each “joining” the vein pipes get progressively larger and larger. The larger dominant veins get bestowed with names!
SUPERFICIAL VEINS VS. DEEP VEINS:
Veins that are located in the central portion of the leg are called deep veins. Veins that are located close to the skin surface are called superficial veins.
Major superficial veins in the leg:
Great Saphenous Vein (GSV) – Starts near the inner ankle. Runs up the inner calf & thigh. Terminates in the groin (by joining with deep vein)
Anterior Accessory Great Saphenous Vein (AAGSV) – Runs up the front portion of the thigh. Terminates by joining with the upper portion of Great Saphenous Vein
Posterior Accessory Great Saphenous Vein (PAGSV) – Runs up the inner part of the thigh. Terminates (by joining with the upper portion of Great Saphenous Vein)
Small Saphenous Vein (SSV) – Starts near the outer ankle, runs up the back of the calf. Terminates behind the knee (by joining with deep vein)
Major deep veins in the leg:
Common Femoral Vein – located in the groin area
Femoral Vein (in the thigh) – runs from lower thigh to groin
Popliteal Vein – runs from upper calf to behind the knee
Anterior Tibial Vein(s) – located in the calf
Posterior Tibial vein(s) – located in the calf
Peroneal Vein(s) – located in the calf
Gastrocnemius Veins – located in the calf
Soleal Veins – located in the calf
WHY ARE VEINS BLUE?
It’s common in anatomy textbooks for arteries to be depicted as “red”, and veins to be depicted as “blue”. Interestingly, the natural color of both arteries and veins is a fleshy, pale, beige color. The reason why veins appear dark blue-purple is because vein walls are extremely thin, which makes vein walls partially translucent. Dark-red, oxygen-depleted blood within a vein appears blue-purple when visualized through the thin, translucent, beige-colored vein wall and overlying skin.
WHY DO VEINS BULGE?
Venous reflux is the condition where the valves in the upstream leg veins (normally the Great Saphenous Vein or Small Saphenous Vein) have ceased functioning normally. Venous reflux (venous insufficiency) is the underlying condition most commonly associated with varicose veins.
Venous reflux is commonly the consequence of weakening or stretching of the vein wall. When this occurs the flap-like valve leaflets inside the vein cannot come together properly. When the vein valves are not working properly, back-pressure builds up in the vein.
Bulging varicose veins in the leg are, conceptually, like fruit on the ends of branches of an upside-down vein tree. The valves are located in the “trunk” of this vein tree. When these valves stop working, pressure builds up in the trunk. This increased pressure is transmitted to the branches and twigs. The “fruit” on the end of the tree branches (varicose veins) are more likely to bulge and swell when there’s increased pressure within the tree branches.
When veins are under increased pressure they can bulge out through the skin surface, a situation known as varicose veins. Varicose veins can cause symptoms, especially when they are large and bulging. People who have painful bulging varicose veins are nearly always a candidate for vein procedures.
WHY DO PEOPLE GET VARICOSE VEINS?
Quite often the presence of large dilated veins is associated with a family history of varicose vein issues in one or both parents.
In women, pregnancies can put significant strain on the veins due to direct vein compression in the pelvis, exacerbated by hormonal changes that occur during pregnancy.
Other risk factors include increasing age, being overweight or obese, and a sedentary lifestyle.
WHICH VEINS GET AFFECTED WITH VENOUS REFLUX?
The vein that’s most commonly affected with venous reflux is the longest in the body, the Great Saphenous Vein (GSV). This “superficial vein” starts on the inner ankle, runs up the inner leg, and terminates in the groin when the vein joins with the deep venous system. This vein typically lies about 1-4cm below the skin surface, although in some the Great Saphenous Vein (GSV) may lie closer to the skin, or run a deeper course.
The vein second-most commonly affected by venous reflux is the Small Saphenous Vein (SSV). This vein is also considered a “superficial vein”. Venous reflux in the small saphenous vein (SSV) tends to cause symptoms in the lower portion of the leg and ankle.
Venous reflux also commonly affects the Anterior Accessory Great Saphenous Vein (AAGSV).
Venous reflux can also affect the deep veins in the legs, but this is much less common than reflux affecting the superficial veins.
WHAT ARE THE SYMPTOMS?
Some people with spider veins (small skin surface veins <1mm in diameter), reticular veins (small skin surface veins 1-3mm diameter), and small varicose veins (dilated veins >3mm in diameter) may have no symptoms, or only have mild intermittent symptoms.
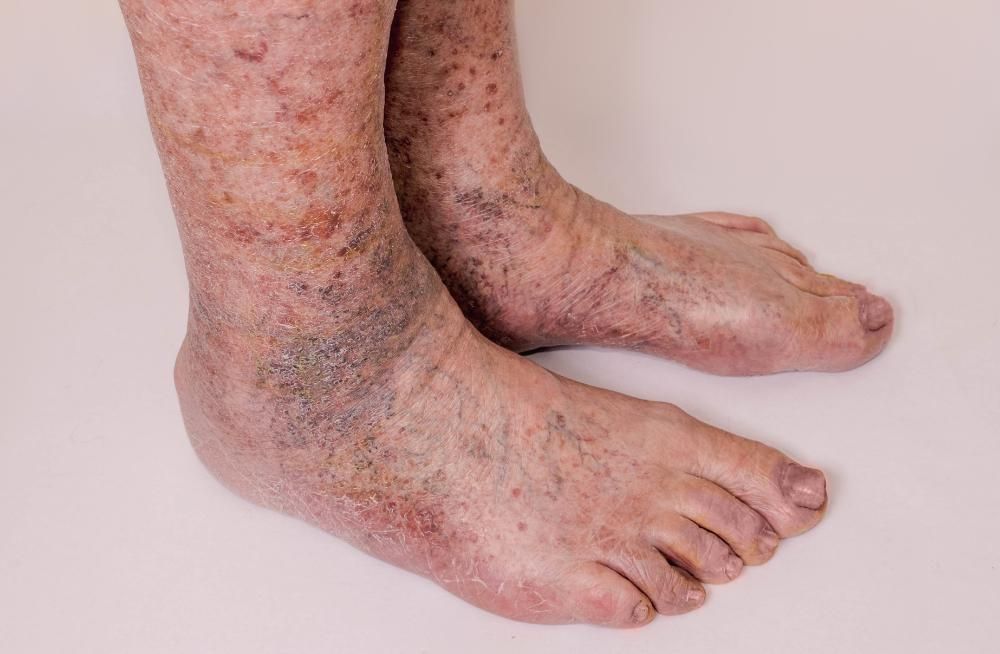
Many people with underlying vein problems will eventually develop leg symptoms. The quality and severity of symptoms are surprisingly diverse. Common symptoms include leg heaviness, early leg fatigue, leg aching, leg cramps, leg restlessness, leg swelling, and ankle discoloration. Less commonly people with venous reflux will develop recurrent skin infections (cellulitis) or skin breakdown (venous ulcer).
Most people with vein related symptoms report that they cannot recall exactly when the symptoms started, reflecting the insidious slow progression of this condition over time.
Vein-related symptoms tend to be exacerbated by prolonged standing, and are commonly worse in hot weather, and towards the end of the day. Paradoxically, many people with vein problems will report that their leg symptoms are also exacerbated by prolonged sitting (eg. sitting at a desk or in a vehicle).
Venous reflux and varicose veins are associated with phlebitis and thrombophlebitis. Phlebitis is a condition where the vein has become inflamed and irritated, generally felt to be incited by stretch-injury to the vein wall. Thrombophlebitis is a related condition where the vein is not only inflamed/irritated, but the clot has also formed inside the vein. Phlebitis treatment is variable and critically depends on whether there is any clot within (or close to) the deep venous system.
Occasionally people with varicose veins will sustain bleeding from the varicose vein. Bleeding from a varicose vein is more likely to happen when the vein is bulging through the skin surface and is also more likely to occur when the skin overlying the vein has become extremely thinned out. Interestingly smaller varicose veins at the skin surface seem to bleed more often than from rope-like varicosities.
WHAT VEIN TREATMENT OPTIONS ARE AVAILABLE?
Vein treatments are designed to reduce or eliminate symptoms (if symptoms are present), improve or maintain the integrity of the skin (reduce the likelihood of progressive skin discoloration, skin infections, and wounds), and improve the cosmetic appearance of the legs.
Vein procedures are predicated on identifying and treating the underlying vein problem that may be causing the veins to bulge and swell and then using one of several treatments to eliminate or seal the bulging veins themselves. If a person simply has small spider veins (and minimal or no symptoms), direct treatment of the spider veins without investigation of underlying problems is a generally accepted strategy.
Many vein treatment procedures work indirectly. By sealing closed "bad" veins in the upstream vein tree, pressure in the varicose veins is reduced, which results in less aching pain, throbbing, cramping, and leg heaviness.
Multiple office-based procedures work by sealing closed “bad” saphenous veins. These procedures include “cauterizing” the target vein with laser or radiofrequency energy (Closurefast), “gluing” the target vein with an adhesive polymer (VenaSeal closure system), vs. injecting a foam product into the target vein (Varithena). Once the underlying problem has been treated attention can then be directed towards the remaining varicose veins and spider veins. Residual bulging varicose veins can be treated by direct removal (phlebectomy) or by injecting foam solution into the vein (sclerotherapy). Tiny skin surface spider veins can often be treated by “zapping” them with a hand-held laser device. Visit our cosmetic consultations FAQ page for more information.
At Vascular Solutions, we pride ourselves on being the best vein specialists in Charlotte and the Carolinas. Contact us today if you would like to be evaluated.
SHARE: